Unfortunately, wisdom is not the only thing that comes with age.
Growing older is a major risk factor for back pain, which is the second most common reason people visit their family doctors, according to the Cleveland Clinic.
By Angela Whitaker
If you’ve suffered from back pain after moving heavy furniture or working in your garden, you might be tempted to blame it on doing too much. But you should know that age-related degenerative changes can occur in the spine as early as your 30s, making you more susceptible to injury and back pain. By age 50, 97% of people will have degenerative changes in the spine detectable on an MRI.
THE AGING SPINE
You can think of the spine like a high-mileage vehicle. Just like a car has many small parts, the spine is made up of many small components that support the body’s weight and allow you to flex, bend, and twist. As time goes by, the spine is more likely to suffer from wear and tear, just as a car is more likely to have parts break down with each passing mile.
The spinal disks in the lower back are often the first parts of the spine to degenerate. These round and rubbery pads act as shock absorbers between the vertebrae, but as we grow older they begin to shrink. This can lead to pain that worsens after heavy physical activity or holding the same posture for a long time. It also can make you more susceptible to several painful spine issues such as:
A HERNIATED DISK: when the outer shell of a disk is cracked and the soft nucleus at the center protrudes through that crack
SPINAL OSTEOARTHRITIS: when joints in the vertebrae rub together due to shrinking spinal disks and cartilage erosion
SPINAL STENOSIS: when the open spaces within your spine narrow, putting pressure on the spinal cord and nerves
WHERE TO START
With proper self-care, most cases of lower back pain improve within six weeks or less. Your treatment can begin at home with:
Activity Modification: Avoid or decrease activities that cause pain, but limit bed rest to two to three days to keep from losing muscle strength. Resume normal activities as soon as possible – but modify them to avoid any painful movements. Be sure to limit long periods of sitting and standing.
A Different Sleep Position: Sleep with a pillow between your knees if you sleep on your side, or lie flat on your back with pillows placed under your knees.
Heat or Ice: Alternate a heating pad with an ice pack to reduce inflammation and pain and increase mobility. Try using ice for the first 48 to 72 hours and then switching to heat.
Over-the-Counter (OTC) Medications:
Pain relievers like acetaminophen and ibuprofen can relieve back pain caused by strained or sore muscles, but they may not be as effective in treating pain resulting from nerve compression or disk problems.

Spine Specialist & Surgeon, Southeastern Spine
Exercise: Muscle strength is important for back support and good posture. Studies show that yoga, walking, and core-strengthening exercises are all effective in easing chronic low back pain. “For back pain, it’s best to maintain an exercise program that’s part of your life, as opposed to sporadic,” says Dr. Jay Jolley, a spine specialist and surgeon with Southeastern Spine.
Improved Posture: Maintaining good posture will reduce pressure on your back. “Stay erect as much as possible,” says Dr. Jolley. “If you have to work at ground level, sit down on a low bench or stool as opposed to stooping over.”
WHEN TO SEE A DOC
While most cases of back pain are mild and improve on their own with self-care, others may require a visit to the doctor or even the emergency room.
See a doctor, if… your mild to moderate back pain lasts longer than four to six weeks or if your acute pain lasts longer than three days. Also, consult a doctor if your back pain is accompanied by:
- intense back pain at night or while lying down and resting
- severe pain that doesn’t improve after a couple of days of self-care
- abdominal pain
- pain that extends down the back all the way to the bottom of the leg
- pain that causes numbness, weakness, or tingling in one or both legs or back
- a history of cancer
- unintentional weight loss
- swelling or redness on the back
Go to the ER, if… you experience back pain with:
- serious trauma such as a bad fall, sports injury, or car accident
- loss of bladder or bowel control
- fever
WHEN THE PAIN WON’T GO AWAY
If your back pain lasts longer than four to six weeks or grows progressively worse, you may need to see a specialist, such as an orthopedist, neurologist, or pain management specialist.
A specialist can conduct a physical exam and run diagnostic tests to identify what’s causing your pain, and then work with you to develop a comprehensive treatment plan. Treatment often begins with prescribed physical therapy, massage therapy, or chiropractic manipulation.

Pain Medicine Specialist, Integrative Pain Services
of Cleveland, A SkyRidge Health Partner
“When it comes to back pain, I always recommend starting with the more conservative treatments first, like physical therapy, home exercises, and chiropractic,” says Dr. Sung Rock Cho, a pain medicine specialist with Integrative Pain Services of Cleveland. “If your pain is unresponsive to these measures, we may proceed to more invasive treatments.”
When people think about pain management, they often first think of medications like opioids or narcotics. Unfortunately, these medications may do more harm than good in the long run. “There’s no one good way to treat chronic pain because it is a multifaceted condition – there are sensory, cognitive, and emotional dimensions,” Dr. Cho says. “It’s generally best to use a multidisciplinary approach utilizing medical, psychosocial, and therapeutic treatment options.”
Many interventional procedures can provide pain relief, and a specialist can determine which one may be best for you. “Pain medicine is anything but ‘shotgun’ therapy,” says Dr. Joshua Hare, a pain medicine specialist with Hamilton Neurosurgery and Spine Center. “With the lower back, there are a number of potential pain generators. It’s essential to get a correct diagnosis so that you can apply the interventions where they are more appropriate.”
If less invasive treatment options have failed, a doctor may recommend:
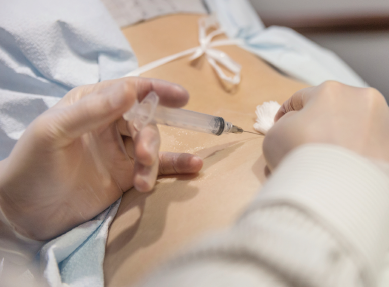 Epidural Steroid Injections. During an epidural steroid injection, a steroid medication is injected into the epidural space of the spine. Steroid injections can be a good option for patients who have back pain in conjunction with a “pinched nerve” or sciatic pain (pain caused by irritation of the sciatic nerve). “These work to reduce inflammation in the tissues surrounding the nerves,” says Dr. Cho.
Epidural Steroid Injections. During an epidural steroid injection, a steroid medication is injected into the epidural space of the spine. Steroid injections can be a good option for patients who have back pain in conjunction with a “pinched nerve” or sciatic pain (pain caused by irritation of the sciatic nerve). “These work to reduce inflammation in the tissues surrounding the nerves,” says Dr. Cho.
Facet Joint Injection. This treatment involves the injection of a steroid medication in the facet joints of the spine. It may be a good option for pain caused by arthritis in the small joints of the back. “These work well for patients with predominantly axial pain (pain confined to one portion of the back),” says Dr. Cho.

Pain Medicine Specialist, Hamilton Neurosurgery and Spine Center, Hamilton Health Care System
Radiofrequency Ablation (RFA) Radiofrequency ablation, in which a radiofrequency device is used to ablate (or essentially “shut off”) nerves transmitting pain signals, is another good option for back pain caused by arthritic joints.
Spinal Cord Stimulation (SCS). Spinal cord stimulation uses an electrical current to treat pain. The electrical pulse interferes with the nerve impulses that make you feel pain. “Patients who have recurrent pain after back surgery often get the most benefit out of spinal cord stimulation,” says Dr. Hare.
Don’t wait!
Although you can’t turn back time and may not be able to escape degenerative spinal changes, proper treatment will usually alleviate the pain and strengthen muscles so you can enjoy life at any age. Don’t suffer in silence if your back pain persists. To determine the most effective back pain treatment for you, consult with your doctor today.
“There are so many options for people with chronic pain and specialists are here to help,” says Dr. Hare. “Our goal is two-fold: to minimize your pain and maximize your function.”
