Is it time to switch up your birth control? Maybe you’ve noticed you’ve gotten more irritable since you started “The Pill,” or maybe you’re using the patch, but you’d rather not have a monthly period. Whatever the reason – if your current method isn’t doing it for you, try another! “Decide what aspects of birth control are a priority for you,” says Mary Helen Durland, nurse practitioner with Women’s Health Specialists. “It’s easier to prevent pregnancy when your birth control method fits your lifestyle and personal preferences.”
To help you better understand your options, we’ve compiled the basics on the major methods of pregnancy prevention that require a doctor’s prescription.
Hormonal IUDs
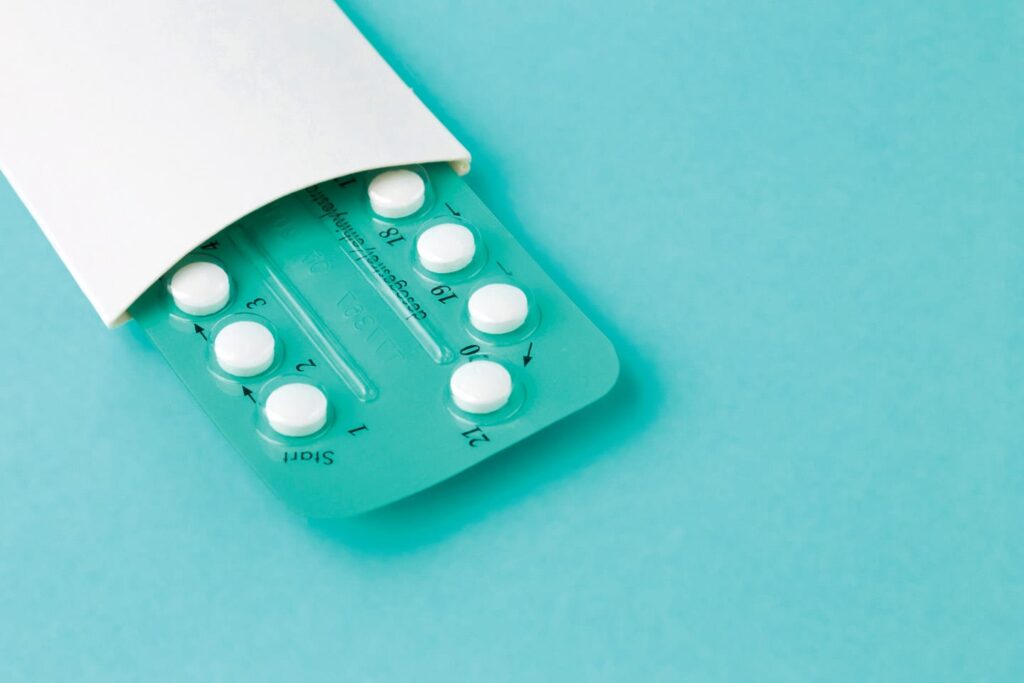
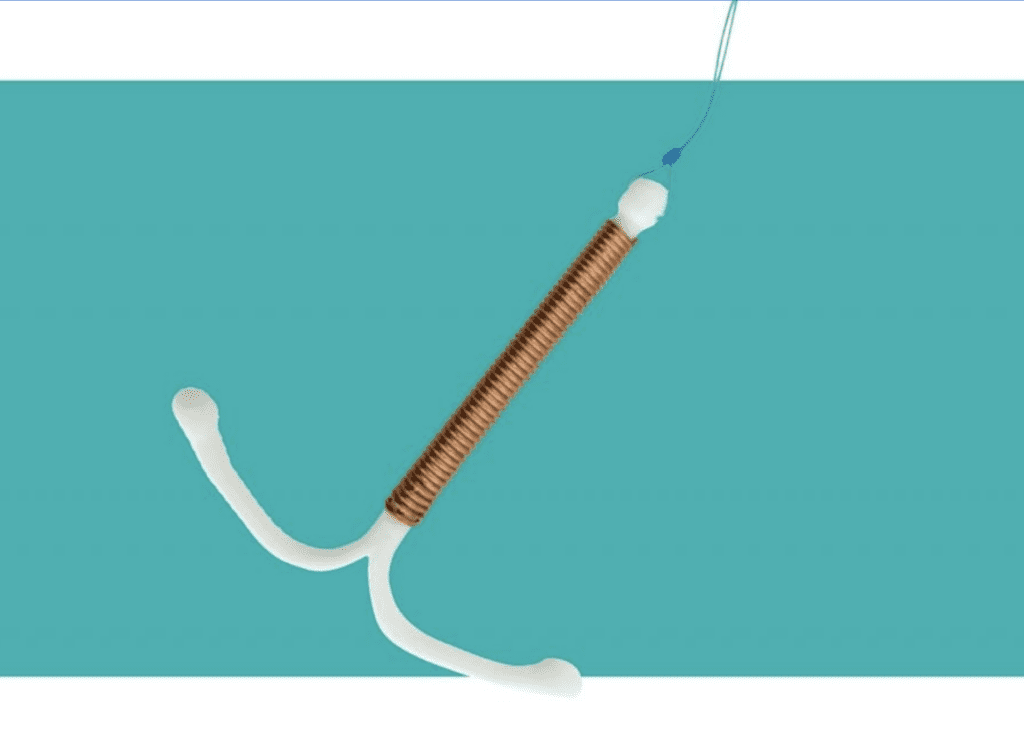
What Is It? A hormonal IUD, or intrauterine device, is a t-shaped, reversible contraception option that lasts 3-5 years. The device is inserted into your uterus through your cervix by your doctor, and a string hangs down to let you know it’s in place. Insertion shouldn’t take more than a few minutes.
Percent Effective: 99%
How They Work: There are currently four hormonal IUDs on the market, and each releases a slightly different amount of levonorgestrel, a synthetic form of the progesterone hormone – Mirena releases 20 micrograms a day, Liletta 19.5, Kyleena 17.5, and Skyla 14. The hormones may prevent your ovaries from releasing an egg, thin your uterine lining, and thicken your vaginal mucus to make it difficult for sperm to find and fertilize an egg.
Should you decide you want to get pregnant, just get the IUD removed, even if it’s early. “After an IUD is removed, a woman’s fertility returns right away, and she can conceive immediately,” says Dr. Sarah Harris, an OB-GYN with Galen Medical Group.
Common Side Effects Include: Light or non-existent periods, nausea, ovarian cysts, spotting between periods, and mood swings; the IUDs that release the greatest concentration of hormones typically lead to more pronounced side effects than those that release the least.
Good Candidates: Women with heavy periods who want ample protection
Bad Candidates: Women who don’t react well to synthetic hormones or are prone to ovarian cysts
Non-Hormonal IUDs
What Is It? The non-hormonal IUD option is called PARAGARD, and it’s wrapped with thin copper wiring. It is inserted the same way as the hormonal versions. This is the longest lasting birth control option, keeping you protected for up to 10 years.
Percent Effective: 99%
How They Work: The copper causes an inflammatory reaction in your body that prevents sperm from reaching and fertilizing an egg. Unlike the hormonal version, the copper IUD does not stop the ovaries from ovulating each month.
Common Side Effects Include: Cramps, heavier and/or longer periods, spotting between periods
Good Candidates: Women with normal to light periods who want to avoid synthetic hormones and want a long-lasting option
Bad Candidates: “Women with very heavy or painful periods should avoid the copper IUD, as it can worsen symptoms,” says Dr. Harris.
Myth Busting
Though IUD usage has significantly increased in recent years, there is still some misinformation out there. Dr. Shevonda Sherrow, OB-GYN with Innovative Women’s Health Specialists, explains, “In the 70s, an IUD came on the market, and its strings caused infections. It wasn’t on the market for very long, but people still to this day think an IUD will give you an infection or make you infertile. That’s simply not true.”
Implantation Rod
What Is It? Better known by its brand name, NEXPLANON, this matchstick-sized rod is inserted into your upper arm by your doctor. Once implanted, you don’t have to worry about it again for a while, since it protects against pregnancy for up to 3 years.
Percent Effective: 99%
How It Works: The rod releases a steady dose of progestin, which thickens the mucus on your cervix making it harder for sperm to reach eggs. The progestin also often stops your ovaries from releasing eggs entirely.
If you decide you want to have children before the 3 years is up, your doctor can remove it early with no long-term side effects.
Common Side Effects Include: “The most common side effect of the implant is unpredictable bleeding,” says Durland. “Other potential side effects are usually associated with hormone use, such as headaches and weight gain.”
Good Candidates: Women who want long-term protection without having to follow a daily routine
Bad Candidates: Women with unexplained vaginal bleeding, history of blood clots, or current or past history of breast cancer
Injections
What Is It? Given every 3 months, Depo-Provera is an injection that protects against pregnancy. It contains progestin but no estrogen.
Percent Effective: 94%
How It Works: Your doctor will administer the shot into your arm once every 3 months. The shots contain progestin, and therefore stop the ovaries from releasing eggs and thicken the cervical mucus to keep sperm from reaching eggs.
Common Side Effects Include: Spotting, headaches, weight gain, loss of bone density, dizziness
Good Candidates: “Women who desire a convenient, discrete contraceptive that requires administration only 4 times per year or women who need an option that doesn’t contain estrogen may be interested in the injections,” says Dr. Harris.
Bad Candidates: Women who want to get pregnant quickly after getting off birth control – this method can take over 1 1/2 years to wear off entirely in some women.
Oral Contraceptives
What Is It? You likely know it as “The Pill,” and it comes in a number of brands that each contain different concentrations of hormones. Some contain both estrogen and progestin, while others are progestin-only (known as “mini-pills”). There are also options that decrease the frequency of your period, or eliminate it altogether. It is safe, affordable, and effective, but you have to remember to take it at the same time every single day. Missed or late pills – even just one – can result in pregnancy.
Percent Effective: 91% (due to human error)
How It Works: The hormones stop your ovaries from releasing an egg and thicken the mucus on the cervix, making it harder for sperm to locate and fertilize eggs.
Common Side Effects Include: Spotting, nausea, breast tenderness, headache, water weight gain, and decreased libido. “The nausea and weight gain should dissipate within the first 3 months, but decreased libido can persist,” says Dr. Sherrow.
Good Candidates: Women with irregular or heavy periods, major PMS symptoms, acne, and a proneness to ovarian cysts
Bad Candidates: Women who may have trouble sticking to the daily regimen, those with hypertension, those prone to blood clots, and those with current or past history of breast cancer
Patch
What Is It? With this method, you apply a contraceptive patch to your stomach, upper arm, bottom, or back once a week for 3 weeks, followed by one week off, in which you will experience your period. These patches contain higher levels of estrogen than oral contraceptives.
Percent Effective: 91% (due to human error)
How It Works: The hormones in the patch stop your body from ovulating and thicken the mucus on your cervix. Your body absorbs the hormones in the patch through your skin.
Common Side Effects Include: Spotting, nausea, breast tenderness, headache, and skin irritation
Good Candidates: Women with irregular or heavy periods, major PMS symptoms, acne, and a proneness to ovarian cysts
Bad Candidates: Women who may have trouble sticking to the weekly regimen, as well as those over 35 who smoke or are prone to blood clots

“Talk to your doctor if you’re unhappy with your current method. They can help address specific concerns so that you find the best option for your lifestyle.”
Dr. Sherrow
Vaginal Ring
What Is It? Known as the NuvaRing, this small, flexible ring is inserted into the vagina to prevent pregnancy. Women who use the ring can either place the ring for 3 weeks, remove it and take 1 week off (where she’ll have her period), then place a new ring, or she can skip periods altogether and replace every 4 weeks.
Percent Effective: 91% (due to human error)
How It Works: The NuvaRing releases estrogen and progestin into the vaginal lining, stopping ovulation and thickening the mucus on the cervix to make it more difficult for sperm to reach and fertilize eggs. And according to Durland, “The vaginal delivery of hormones allows a lower total hormone dose than oral contraceptive pills.”
Common Side Effects Include: Spotting, vaginal discharge, nausea, mood changes, and breast tenderness
Good Candidates: Women with heavy or painful periods, those looking for an easy method that can be self-administered
Bad Candidates: Women over 35 who smoke, those who are prone to blood clots, those with hypertension, those who have had a stroke, and those with current or past history of breast cancer

Mary Helen
Durland Nurse Practitioner, Women’s Health Services

Dr. Shevonda Sherrow
OB-GYN, Innovative Women’s Health Specialists

Dr. Sarah Harris
OB-GYN, Galen Medical Group




