Painless Procedures for Varicose and Spider Veins
Varicose veins and spider veins are considered some of the most chronic conditions in North America. Roughly 50 to 55 percent of women and 40 to 45 percent of men in the United States suffer from some type of vein problem. Varicose veins affect half of all people 50 years and older. Since the beginning of written history, humans have suffered from varicose veins. In ancient history, vein treatments could be crude and painful. Fortunately, treatment methods have undergone major medical advances in the last 2,000 years. Today, simple and virtually painless treatment options offer renewed vitality to those who suffer from varicose and spider veins.

Causes & Symptoms
In simple terms, the arteries are responsible for carrying blood from the heart to the body, and the veins return the blood to the heart. All veins have one-way valves that regulate blood flow. As the heart pumps, blood moves through the veins and then the valves shut to prevent blood from flowing backward.
According to Dr. James Morrow, a board certified interventional radiologist with Tennessee Imaging and Vein Center in Chattanooga, veins have a harder job to accomplish than arteries. “Veins have to work against gravity, pushing upward toward the heart,” he says. “That is why veins are particularly susceptible to venous disease.”
When a vein wall becomes weak or damaged, or if the valves are injured or stretched, blood can leak backward toward the foot, which is called reflux. Over time, this leaking can lead to higher pressure in the veins, which can cause a variety of venous disease disorders, including varicose and spider veins.
There are three types of veins in the legs: superficial veins, communicating veins and deep veins. Typically, varicose and spider veins occur in superficial veins called the great saphenous and small saphenous veins.
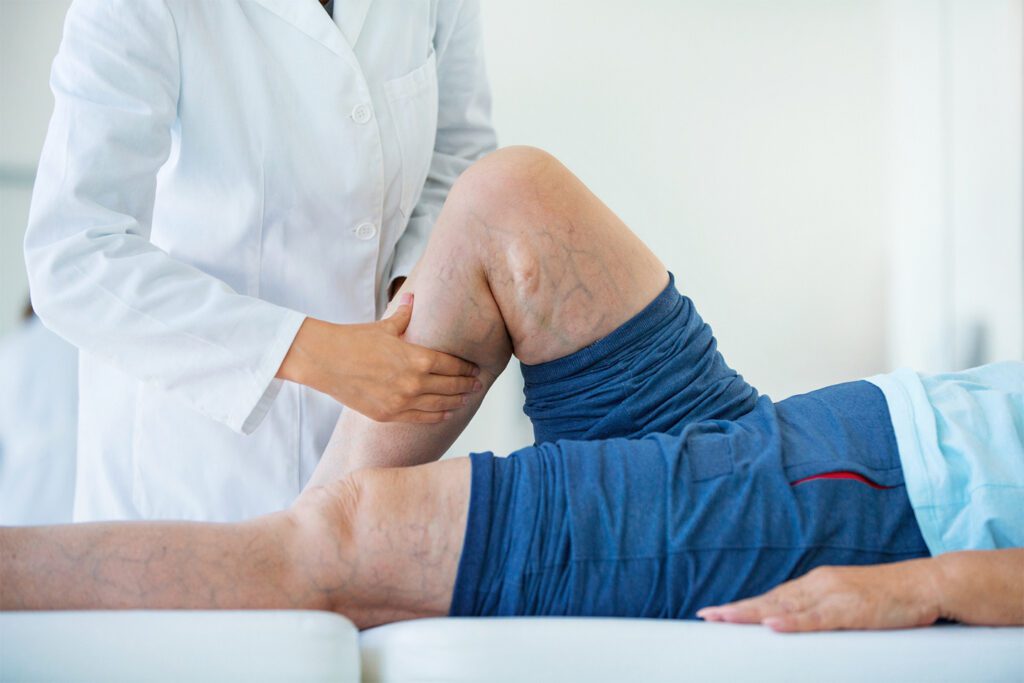
Spider veins are the small blue to red blood vessels that lie close to the surface of the skin, appearing in lines or web-like patterns. Typically, spider veins appear on the thigh, calf and ankle, but they can also appear around the nose and lips. Spider veins, medically known as telangiectasias, are dilated capillary veins less than 2 mm in diameter. Spider veins are usually only a cosmetic concern and are generally medically insignificant. Varicose veins are the dilated and twisted blue veins that bulge beneath the skin. Typically ½-inch or larger in diameter, they can occur anywhere in the leg from the groin to the ankle.
Risk factors for varicose veins and spider veins include:
- Increasing age: With age, vein valves may weaken.
- Medical history: Approximately half of all people who have varicose veins have a family member who has them, too.
- Hormonal changes: Puberty, pregnancy and menopause can cause vein changes. Birth control pills and other medicines containing estrogen and progesterone also may contribute to the forming of varicose or spider veins.
- Pregnancy: The amount of blood in the body increases, causing veins to enlarge. The growing uterus also puts pressure on veins.
- Obesity: Being overweight or obese can put added pressure on veins.
- Lack of movement: Sitting or standing for a long time forces veins to work harder to pump blood to the heart. Sitting with legs bent or crossed can also create problems.
- Sun exposure: Too much sun can cause spider veins on the cheeks or nose.
Varicose veins can cause a variety of symptoms. Mild symptoms can include heaviness, burning, aching and cramps. These symptoms can increase after sitting or standing for long periods of time. More serious symptoms can include leg swelling, leg tiredness and pain. As the condition worsens, skin changes (color changes, dry and thinned skin, inflammation and scaling) and leg ulcerations can also occur.
Dr. Griffin Coates, a board certified cardiac and thoracic surgeon with Vein Therapies of Chattanooga, says that many people endure the symptoms of varicose veins for years because they can be subtle; however, treatment can make a tremendous difference in quality of life.
“Because of a heredity factor and hours and hours of standing, I developed varicose veins,” says Dr. Coates. “I had been denying the symptoms, but after receiving treatment I felt like pounds had been taken off my legs. There are a lot of other health benefits to treating varicose veins, including the increased ability to exercise.”
Treatment Options
In the past, painful procedures prevented many people with varicose and spider veins from seeking treatment. However, treatment options have undergone enormous advances in recent years. Today, there are a variety of outpatient procedures available that are virtually painless and offer quick recovery.
Drs. Morrow and Coates both recommend that patients receive an initial medical evaluation for problems with varicose or spider veins. Many doctors will conduct an ultrasound to look at a patient’s vein structure, check blood flow and look for blood clots. Occasionally, a venogram will be performed, which offers a more detailed look at blood flow through the veins.

Many doctors suggest compression socks to relieve some of the symptoms of varicose veins and help move blood more efficiently through the legs. Although wearing compression socks will not eliminate varicose and spider veins, they can help alleviate symptoms and prevent worsening. Women who are pregnant and people who are on their feet all day long are good candidates for compression socks, as well.
For people with mild symptoms, Dr. Morrow recommends over-the-counter compression socks, which come in 10-15 mmHg and 15-20 mmHg. Additional strengths can be ordered with a prescription. Compression socks can be purchased at surgical supply stores, some pharmacies and online.
Most medical treatments for varicose and spider veins are designed to heat and destroy damaged veins. According to Dr. Morrow, this is not problematic for the human body, which has more than enough veins to make up for any faulty ones. “The body has all kinds of alternate connections, so when one pathway is closed, the body just reroutes the blood to other healthy veins,” he says.
The following treatment options are available today for varicose and spider veins:
Radiofrequency Occlusion
An outpatient procedure that uses a small catheter, which is inserted into the vein. The catheter delivers a radiofrequency energy to the vein wall, causing the collagen in the wall of the vein to shrink and the vein to close. Once the diseased vein is closed, blood is re-routed to other healthy veins. Following the procedure, walking is encouraged and compression stockings should be worn during the day for two weeks.
Dr. Coates is a proponent of the VNUS Closure Procedure, a 45-60 minute outpatient radiofrequency occlusion procedure. “I think the VNUS method is the best because it is virtually painless and patients can get back to work and exercise immediately,” he says.
Endovenous Laser Treatment
An outpatient procedure that uses a small laser fiber inserted into the vein. Pulses of the laser light are delivered into the vein, causing it to collapse.
Tennessee Imaging and Vein Center offers a laser treatment called VenaCure, a minimally invasive procedure that uses a laser to “weld” the vein closed. This 45-minute outpatient procedure requires only local anesthetic, which Dr. Morrow says makes the procedure painless. Patients are up and walking as soon as the procedure is over and can return to normal activity. Compression hose are worn for two weeks following treatment.
“I usually let my patients decide if they want to use VNUS Closure radiofrequency occlusion or laser treatments,” says Dr. Morrow, whose office offers both procedures. “The only difference is the way in which the vein is heated.”
Sclerotherapy
Also known as injection therapy, is a nonsurgical medical procedure used to treat varicose veins and spider veins. A tiny needle is used to inject a sclerosing solution directly into the vein. The solution irritates the lining of the vein, causing it to swell and stick together and the blood to clot. Over time, the body absorbs the treated vein.
Dr. Robert Magill, co-owner of Larimar Medspa, says, “sclerotherapy can be done with minimal discomfort to the patient. The treatment time depends on the amount of veins that need to be treated, and it is not uncommon to require several treatments for optimal results. After treatment, patients can immediately return to non-impact/non-stressful routine daily activities. Compression stockings are recommended to assist in inhibiting the return of/or development of unsightly veins.”
Surface Laser Treatments
Surface lasers or intense pulsed light treatments are used to heat and selectively damage or destroy spider veins and smaller varicose veins. No needles or injections are required; however, the heat from the laser can cause some pain. Laser treatments last for 15 to 20 minutes and, generally, two to five treatments are needed to remove spider veins in the legs. Laser therapy usually isn’t effective for varicose veins larger than 3 mm.
If needed, the following surgical procedures can be used to treat large varicose veins:
Ambulatory Microphlebectomy
The surgical removal of surface varicose veins. Using specially designed instruments, the abnormal vein is removed through tiny punctures in the skin. This minimally invasive procedure uses local anesthesia and does not require stitches. Discomfort is minimal and a bandage and/or compression stocking is worn for a short period of time following the procedure.
Surgical ligation and Stripping
A surgery that involves tying shut problem veins and completely removing them from the leg through small cuts in the skin. This surgery requires general anesthesia and must be done in an operating room. Recovery takes one to four weeks and pain in the leg is the most common side effect.
PIN stripping
A surgical procedure in which an instrument called a PIN stripper is inserted into a vein. The tip of the PIN stripper is sewn to the end of the vein and the vein is pulled out. This procedure can be done in an operating room or outpatient center with general or local anesthesia.
Many insurance companies will cover the cost of treating varicose veins, but generally not spider veins. The best approach is to check with the insurance company for coverage before considering treatment options.
Prevention
According to the National Women’s Health Information Center, the following steps can help reduce the chance of getting varicose and spider veins and ease the discomfort of any existing problem veins:


- Wear sunscreen to protect skin and limit spider veins on the face.
- Exercise legs regularly through walking or running to improve leg strength, circulation and vein strength.
- Control weight to avoid excess pressure on leg veins.
- Don’t sit with your legs crossed for long periods of time. Elevate legs when resting as much as possible.
- If standing for long periods of time, shift your weight from one leg to the other. If sitting for long periods of time, stand up and move around every 30 minutes.
- Wear compression socks or stockings during the day and avoid tight clothing that constricts the waist, groin or legs.
- Avoid wearing high heels for long periods of time. Lower-heeled shoes help tone calf muscles and help move blood through the veins.
- Eat fiber to reduce constipation, which can contribute to varicose veins. Eating less salt can help prevent swelling that comes with varicose veins.
Although incidence rates for varicose and spider veins are high, treatment options today can offer relief and a better quality of life to those who suffer from unsightly and painful veins. “Treating varicose veins can make a tremendous difference in how someone looks and feels,” encourages Dr. Coates. “There are so many positive health benefits that result, aside from just treating the varicose veins.”
Dr. James Morrow
Board Certified Interventional Radiologist, Tennessee Imaging and Vein Center in Chattanooga
Dr. Griffin Coates
Board Certified Cardiac and Thoracic Surgeon with Vein Therapies of Chattanooga

